

Pulse oximetry and
BluPRO

What is a Pulse Oximeter?
The pulse oximeter is a device that continuously measures the oxygen saturation in arterial blood (how much hemoglobin is bound to oxygen) without blood sampling. The principle of pulse oximetry was invented by Dr. Takuo Aoyagi, an engineer at Nihon Kohden in 1972. To read more story about Dr. Aoyagi, visit our Global Website.
Use of Pulse Oximeters
The pulse oximeter is a device that continuously measures the oxygen saturation in arterial blood without blood sampling. The pulse oximeter has been popularized for respiratory management in the perioperative period and in ICUs, but with the advent of smaller devices such as the transmitter and hand-held types, its use has expanded to outpatients and hospital wards.
Today, the probe and main unit have been miniaturized and are widely used outside of hospitals, including for home care. SpO2 has also been used as an evaluation criterion in classifying the severity of COVID-19 infection, making it an increasingly indispensable vital sign.
Operating Room
Recovery Room
Oxygenation assessment after anesthesia in the perioperative period
ICU
- Respiratory management under ventilation
- Weaning index
- Respiratory management of patients with sedatives or analgesics
NICU
- Detection of hypoxemia
- Oxygen management to prevent retinopathy of prematurity
Wards
- Vital sign monitoring by SpO2 and pulse rate
- Spot check monitoring of oxygen levels during rounds
Emergency Room
Management of oxygen administration
Laboratory
Detecting hypoxemia during tracheal stroscopy or endoscopy
Home care
- Determination and prescription of home oxygen therapy
- Respiratory management
- Screening of Sleep Apnea Syndrome
The Principle of Pulse Oximetry
SpO2 is the arterial blood oxygen saturation measured transcutaneously with a pulse oximeter, which quantifies the percentage of hemoglobin that is bound to oxygen in the red blood cells of arterial blood.
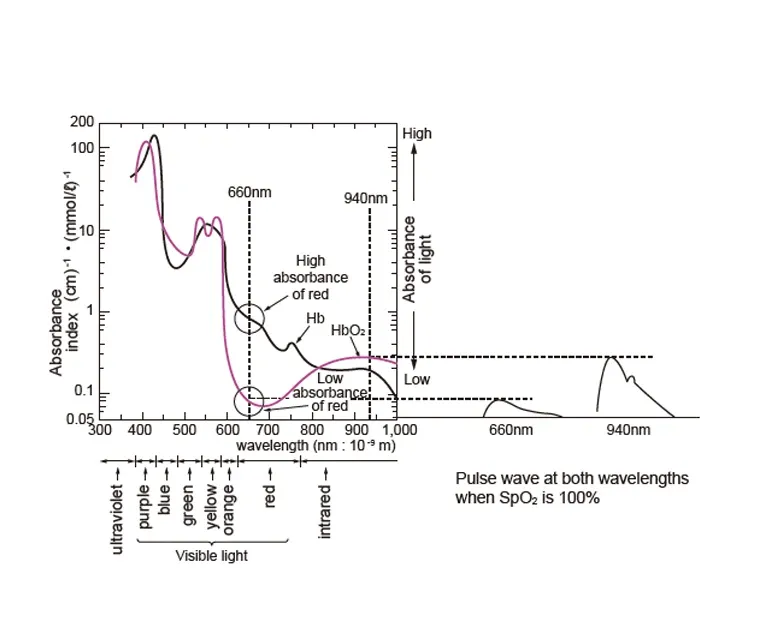
Hemoglobin turns bright red when bound to oxygen, and it turns dark red when unbound. The oxygen saturation of arterial blood is calculated by utilizing the fact that the ease of absorbing light differs depending on the color. Two types of light of the small devices attached to the fingertips of the hand, and the sensor on the other side measures the light that passes through the finger without being absorbed and analyzes it.
- A probe with two LEDs (660 mm for red light and 940 mm for infrared light at Nihon Kohden) is attached to a part of the body with relatively thin tissue, such as a finger or toe.
- A photo detector detects the two wavelengths that pass through the measurement site and calculates the oxygen saturation of arterial blood from the pulse wave, absorbance and amount of blood obtained from the 2 signals.
Reference
1) [Improvement of Earpiece, oximeter] (in Japanese). Japanese Society for Medical and Biological Engineering Abstract. 12, 90-91, 1974.
2) [The Birth of the Pulse Oximeter and its Theory] (in Japanese). The Journal of Japan Society for Clinical Anesthesia. 10(1), 1-11, 1990.
3) [Pulse Oximetry and Its Simulation] IEEE Tokyo Section Denshi Tokyo. 29, 184-186, 1990.
4) Takuo, Aoyagi. [Theoretical and Experimental Investigations of Blood Dimming] (in Japanese). Japanese journal of medical electronics and biological engineering : JJME. 30(1), 1-7, 1992.
Nihon Kohden's SpO2 Measurement Technology, the NPi Algorithm
SpO2 algorithm with enhanced artifact prevention, NPi
The NPi algorithm is Nihon Kohden’s unique filtering function to effectively remove artifacts. Its features include the extraction of the pulse wave fundamental frequency using a coordinate-transform method and frequency analysis, and artifact removal using a narrow-band filter based on the extracted fundamental frequency.
Basic processing of SpO2 measurement
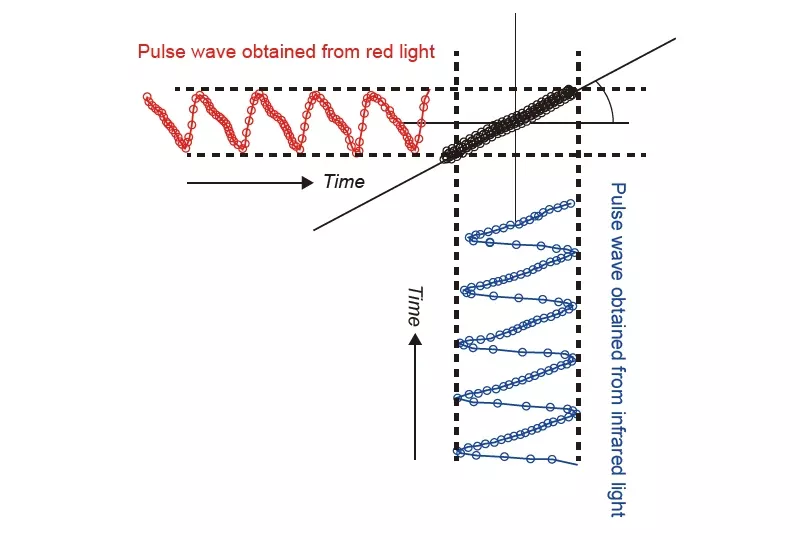
SpO2 is calculated from the amplitude ratio Φ of the pulse waves of two wavelengths of red and infrared light emitted by LEDs. Nihon Kohden’s pulse oximeter plots the pulse wave signals of infrared light and red light on the XY coordinate axes as shown in Figure 1 and calculates Φ from the slope of the regression line obtained by the least square method. Since this method uses all of the waveform data, it enables more accurate calculation of Φ than the method that uses only the maximal and minimal amplitude.
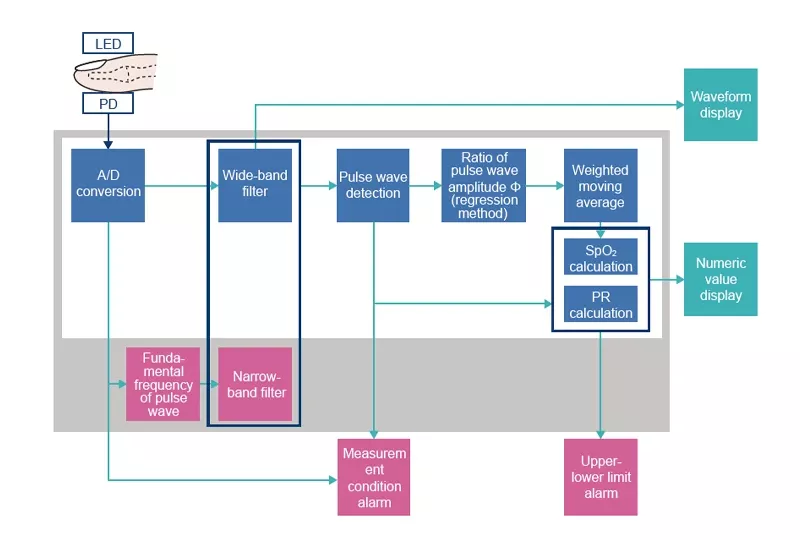
NPi algorithm
The NPi algorithm enhance the filtering function that removes artifacts from the pulse wave while maintaining the basic processing of the conventional algorithm. Its characteristic features are the extraction of the fundamental frequency of pulse wave by frequency analysis (Figure 2) and the removal of artifacts using a narrow-band filtering based on that frequency analysis. This function is especially effective when there are relatively large artifacts in the pulse wave amplitude, such as when a patient with peripheral circulatory failure becomes restless, or in the case of respiratory variation with neonates.
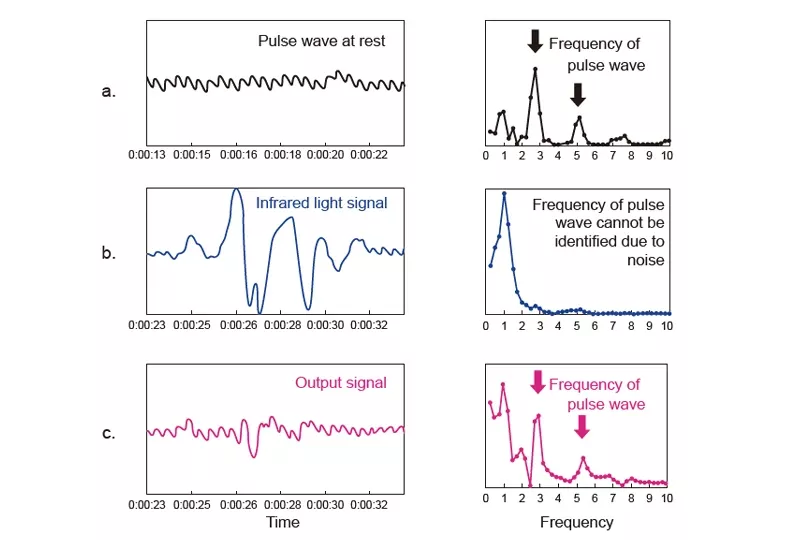
Pulse waves have a fundamental frequency that is the same as the pulse rate and a frequency component that is a constant multiple of this frequency (Figure 3). When performing frequency analysis of a waveform with a large superimposed artifact, it is difficult to identify the pulse wave frequency because the pulse wave signal gets lost in the artifact (Figure 3b). Even in such situations, using Nihon Kohden’s original coordinate-transform method improves the discrimination between pulse wave and artifacts.
Frequency analysis of the pulse wave signal obtained by separating it from the artifact with this coordinate-transform method allows the frequency of the pulse wave to be identified (Figure 3c).
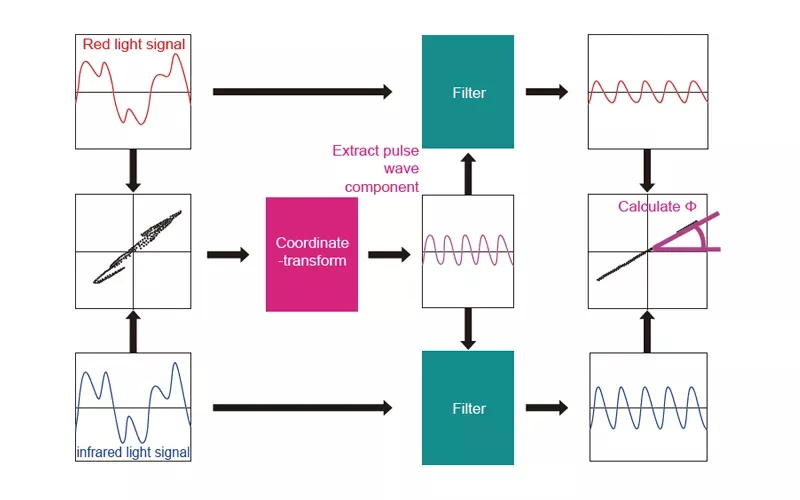
Based on the pulse wave signal obtained by separating it from artifacts with the coordinate-transform method as shown in Figure 4, a narrow-band filter (patented) is used to filter out signals affected by artifacts to accurately extract signals and calculate the pulse wave signal’s Φ.
This method has long been known in the world of signal processing technology, but its application to pulse oximeters has made it possible to accurately separate artifacts from signals and provide highly reliable SpO2 values.
Material Downloads―BluPRO
Learn more

Performance Digest

Pulse Oximeter Accuracy Study






